The pressure on the healthcare sector is a well-known problem which can be attributed to various reasons. Stress could be the consequence of, for example, having saved money on support services. As a result of this practice, there is a high feeling of responsibility for the healthcare workers to take care of the patients themselves [1]. This is especially true now, during the Covid-19 pandemic. Experiencing a lot of stress during work can result in negative effects on health and well-being for both the employees and their patients. This blog post discusses the causes of the high work pressure and stress within the healthcare sector, and the importance of achieving sustainable employability to, in turn, reduce the burden on the healthcare workers.
Causes of pressure
Multiple factors are causing high pressure within the healthcare sector. Regardless of the Covid-19 pandemic, healthcare workers have generally higher risks of feeling depressed, expriencing anxiety, or having a burnout [3]. A cause for this is that there is a growing demand for care due to, for example, the ageing population [2]. Since the employees within the healthcare sector have not increased as much compared to the demands of the ageing population there is a staff shortage [2].
Working as a care worker can be emotionally demanding. This can lead to the risk of employees bringing home the mental and emotional challenges faced at work [2]. On top of that, care workers might feel a higher responsibility compared to other workers from other sectors [2]. Healthcare workers might feel responsible for both their patients and for their colleagues. For example, they feel more responsible for executing their tasks well, as it has a direct impact on the health and well-being of their patients. Plus, when healthcare workers call in sick or do not execute their tasks well, it burdens their colleagues [2].
A last important thing to mention is that healthcare workers must be flexible. They have to work in different working conditions and have a low possibility to organize their work themselves [2]. They have to adapt to irregular working hours [2], as care for people is always needed, day and night. Therefore, they have heavy workloads [3].
Thus, as working in this sector is already a burden in general, the Covid-19 pandemic made things even worse. Coronavirus put extra pressure on the whole healthcare sector. A lot of people got ill, and there were few spaces left in the hospitals, especially at the intensive care department. In general, healthcare workers had to work more hours due to sick people, also amongst their colleagues. On top of that, during a period within the Covid-19 pandemic, elderly care homes were closed, and there were limited visitors allowed in hospitals. This resulted in extra pressure for healthcare workers to feel responsible to be there for their patients/clients/elderly residents, etc. An article in the Philadelphia Inquirer mentioned healthcare workers were put in painful roles as they ‘‘suddenly found themselves as proxies for family, standing by the bedside of patients in their last moments so they didn’t die alone’’ [3]. One can imagine, this results in both extra working hours and emotional burdens.
Regardless of the Covid-19 pandemic, healthcare workers have generally higher risks of feeling depressed, experiencing anxiety, or having a burnout.
Negative health and well-being consequences
As mentioned above, the pressure on the healthcare sector results in negative consequences for the health and well-being of both the employees and the patients. The staff shortage, emotional burdens, feelings of responsibility, heavy workloads, irregular working hours, and the Covid-19 pandemic, all result in feelings of high pressure on this sector. Therefore, healthcare workers might experience more anxiety, depressed feelings, or even a burnout [3]. This also makes it less attractive to work within the healthcare sector, while there already is a shortage of employees. The high pressure might also lead to people valuing their job less. These negative effects will decrease the health and well-being of the healthcare employees, which again puts higher pressure on this work sector. These problems are an ongoing cycle, which needs attention.
Furthermore, when healthcare workers feel more stress, and make more mistakes, this can result in less patient satisfaction [4]. On top of that, when healthcare workers often call in sick, are less productive, value their work less, and have higher intentions to leave their job, it does not contribute to anyone. When people value their work, this has multiple positive consequences. For example, people feel mentally healthier, take fewer sick days, have fewer intentions to leave, and are generally more productive [7]. Healthcare workers valuing their work is of importance. For an organization, it is important to keep the employees working for them and keeping them as healthy as possible. This is referred to as sustainable employability: ‘‘creating the right conditions for employees to have a long, healthy and happy career. By ensuring someone enjoys working, is healthy and motivated, he or she remains employable for a long time’’ [6].
“ […] the pressure on the healthcare sector results in negative consequences […] These problems are an ongoing cycle, which need attention”
How to achieve sustainable employability
To reduce the work pressure and negative effects on the healthcare workers, it is crucial to create sustainable employability in which the healthcare workers value their work. This is a difficult thing to do, as what people value of a job varies depending on personal preferences. Staying healthy also starts by the employees themselves [2]. An unhealthy behaviour of healthcare workers should be changed, although changing behaviour is complicated [2]. Therefore, for an organization, it is of importance to promote vitality and resilience to offer employees some help [2].
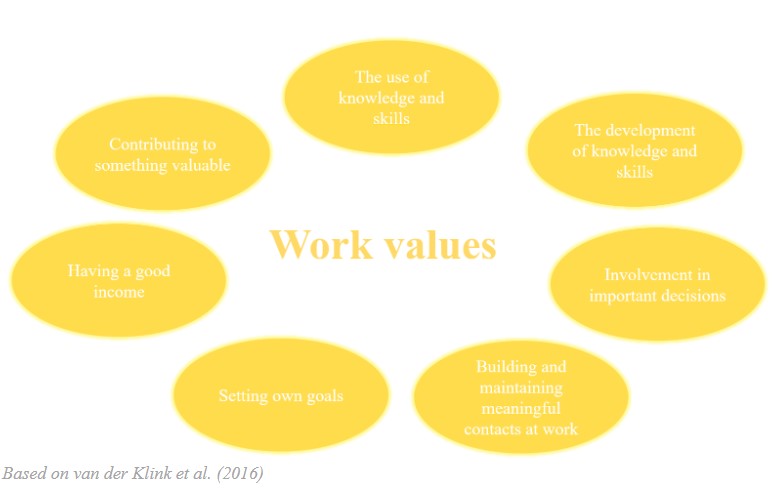
The work value intervention is a practice that focuses on value to promote wellbeing and work engagement [7]. The work value intervention consists of different steps from meetings with the department, to a team intervention [7]. Here, opportunities are given to worker to let them realize what they value the most within their jobs [7]. Research about sustainable employability defined seven work values as shown in the figure below [5]. These work values can also be seen as capabilities. Capabilities refer to the opportunity and ability to achieve people’s most important work values [5]. Here, it is important to consider people’s characteristics as well as external factors (e.g. the working environment) [5]. Organizations should be trained to provide opportunities for employees to create a work environment in which they can achieve their important values. This can be readily achieved with conversations with their employees [7]. Workers should be asked, about each value as shown in the figure below. For example, to what extent the employee thinks the value is important, whether the organization offers the opportunities to achieve the value, and to what extent he or she realizes the value in his/her work [5]. When applying it to the example of healthcare workers, these conversational practices can help discover what they find important within their work, how they can achieve this, and what they can do themselves [7].
“[…] sustainable employability should be promoted within organizations, and conversations with the employees should be started to break this ongoing negative spiral!”
To conclude, the high pressure on the healthcare sector is resulting in negative consequences for its employees, as well as for the patients. This leads to negative effects on the health and wellbeing of the healthcare workers, as well as it might reduce the extent to which they value their job, which might result in again: more pressure. To cope with these problems, sustainable employability should be promoted within organizations, and conversations with the employees should be started to break this ongoing negative spiral!
References
[1] Houwelingen, H., & Wildenborg, F. (2017). Verpleegkundigen staan stijf van de stress. Algemeen Dagblad. Retrieved from https://www.ad.nl/binnenland/verpleegkundigen-staan-stijf-van-de-stress~a854cf20/?referrer=https%3A%2F%2Fwww.google.com%2F.
[2] Minddistrict. (n.d.). Tackling workload stress and absence in healthcare. Retrieved from https://www.minddistrict.com/work-stress-in-healthcare.
[3] Laughlin, J. (2021) As pressure from the pandemic wanes, health-care workers cope with burnout and a fractured community. The Philadelphia Inquirer. Retrieved from https://www.inquirer.com/health/coronavirus/burnout-pandemic-doctor-nurse-mental-health-pennsylvania-new-jersey-20210706.html.
[4] Gärtner, F. R., Nieuwenhuijsen, K., van Dijk, F. J., & Sluiter, J. K. (2010). The impact of common mental disorders on the work functioning of nurses and allied health professionals: a systematic review. International journal of nursing studies, 47(8), 1047-1061.
[5] Van der Klink, J. J., Bültmann, U., Burdorf, A., Schaufeli, W. B., Zijlstra, F. R., Abma, F. I., … & Van der Wilt, G. J. (2016). Sustainable employability—definition, conceptualization, and implications: a perspective based on the capability approach. Scandinavian journal of work, environment & health, 71-79.
[6] Recruit Global Staffing. (2019). This is what sustainable employability means for employers. RGF Staffing. Retrieved from https://rgfstaffing.com/newsroom/n/2019/08/22/this-is-what-sustainable-employability-means-for-employers.
[7] Joosen, Margot. (2021). Lecture: Sustainable employability in healthcare workers. Tranzo Tilburg University.







